Article updated on:
April 15, 2026
DVC Stem employs a dedicated team of medical professionals, tasked with verifying the accuracy of health claims and summaries of medical research. Each member's expertise is aligned with the subject matter of the article to ensure precision and relevance.

Fact-Checked
We evaluate medical studies published in reputable scientific journals to form our opinions on a product or health matter, ensuring the utmost scientific precision.

Medically Cited
Ublituximab vs Ocrevus: Comparison 2026
Learn more about our Stem Cell Treatment
Our treatment protocol is aimed at revolutionizing treatments for degenerative conditions.
50,000+ subscribers
Join our newsletter to learn more about stem cell therapy and the science behind it.
Ublituximab (Briumvi) and ocrelizumab (Ocrevus) are both anti-CD20 monoclonal antibodies for MS, but they differ in infusion time, dosing schedule, and cost. Ublituximab offers a shorter one-hour infusion compared to Ocrevus's longer infusion time, with similar efficacy in clinical trials. Here's a detailed head-to-head comparison.
Key Takeaways
- Understanding the core mechanisms of Ublituximab and Ocrevus in MS management.
- Comparative analysis of efficacy, safety, and cost.
- Insights into patient-centric perspectives regarding these therapies.
- Overview of FDA approval status and availability.
- Delving into the broader spectrum of MS treatment landscape.
Identifying DMT's
Disease Modifying Therapies (DMTs), commonly abbreviated as DMTs, serve as a cornerstone in MS management. They primarily aim at reducing the frequency and severity of relapses, slowing down the progression of disability.
Among the various classes of DMTs, anti-CD20 monoclonal antibodies like Ublituximab and Ocrevus have carved a niche owing to their targeted mechanism in depleting B-cells, a type of white blood cell that plays a pivotal role in the inflammatory processes of MS.
Ublituximab
The recent FDA approval of Ublituximab, now marketed under the brand name Briumvi, has been a significant milestone in the MS treatment paradigm. This therapy operates by targeting the CD20 protein on the surface of B-cells, aiding in their depletion and consequently mitigating the inflammatory responses implicated in MS.
- FDA Approval Status: Ublituximab received FDA approval, paving the way for its use in adults with relapsing forms of Multiple Sclerosis1.
- Mechanism of Action: By honing in on the CD20 protein, Ublituximab facilitates B-cell depletion, a crucial step in curbing the inflammatory cascade associated with MS.
What makes Ublituximab a preferred choice for some patients?
Ublituximab stands out for its more convenient dosing schedule, being administered as a 1-hour intravenous infusion every 6 months. This contrasts with Ocrevus, which requires two separate infusions two weeks apart every 6 months.
Additionally, Ublituximab has demonstrated a potentially faster B cell depletion in clinical trials compared to Ocrevus, indicating a quicker therapeutic response. Another notable advantage is the lower infusion reaction rate associated with Ublituximab, with only 2% of patients in trials experiencing infusion reactions, as opposed to the 34% with Ocrevus, making it a more tolerable option for many individuals.
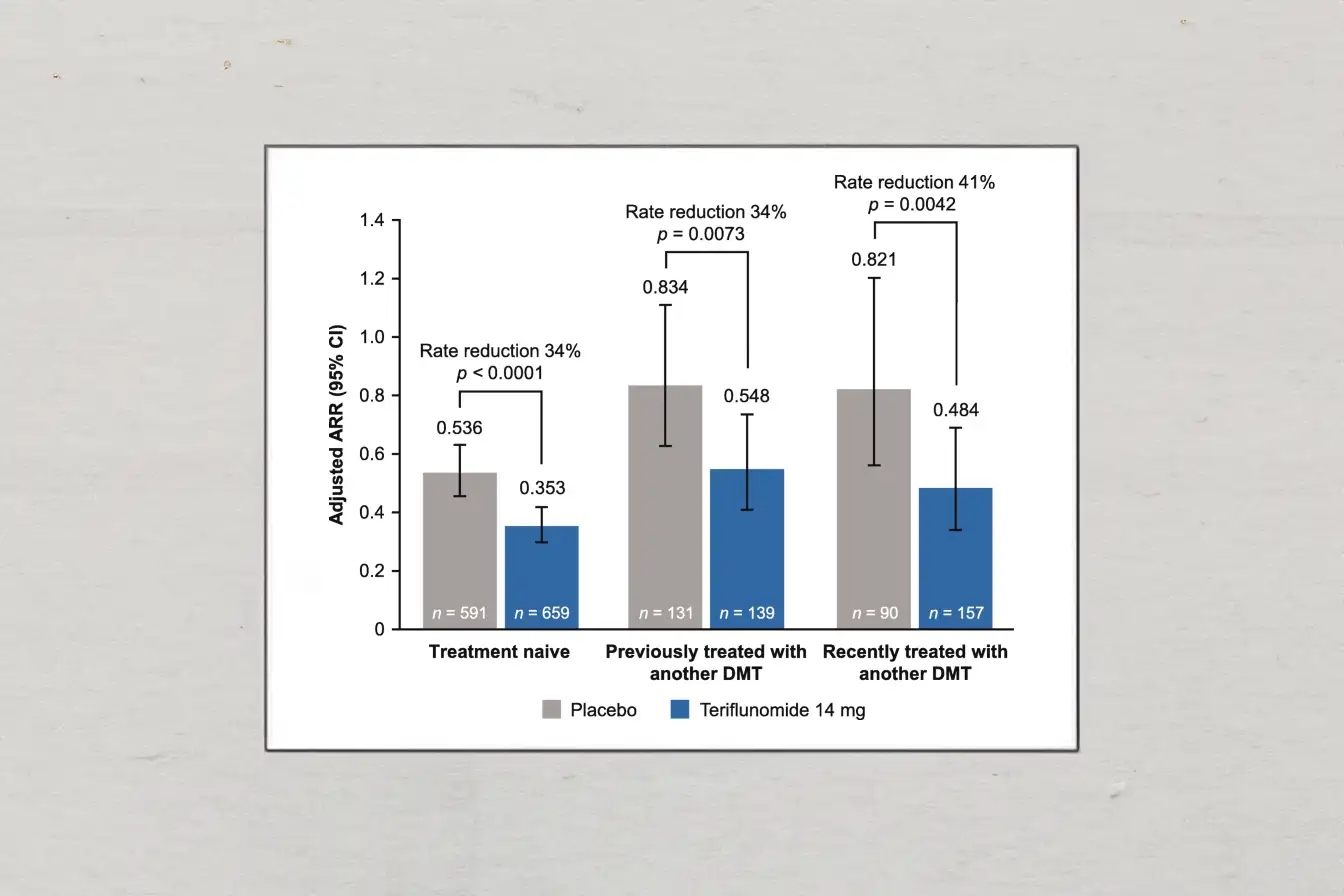
The discourse around Ublituximab and Ocrevus extends beyond the scientific community to resonate with the lives of those affected by MS. It's a narrative of resilience, mirrored both in the relentless endeavors of the scientific community and the daily lives of individuals with MS. As we dissect the efficacy and safety of these therapies, we're also embracing a narrative of hope, which is as therapeutic as the drugs themselves. The pathway towards a cure might still be elusive, but the strides made by therapies like Ublituximab and Ocrevus are not just scientific achievements, but a testament to human resolve.
What are the limitations associated with Ublituximab?
Ublituximab trails behind when it comes to a proven track record. While Ocrevus has been on the market since 2017, Ublituximab is still undergoing clinical trials, rendering long-term safety and efficacy data more robust for Ocrevus.
Moreover, Ublituximab is only available as an intravenous formulation, unlike Ocrevus which also provides a subcutaneous dosing option, limiting its versatility in administration.

Ocrevus
Ocrevus (ocrelizumab), another potent player in the domain of MS treatment, has also been in the limelight for its efficacy in reducing relapse activity in individuals with Relapsing-Remitting Multiple Sclerosis (RRMS). Much like Ublituximab, Ocrevus targets the CD20 protein on B-cells, albeit with its unique formulation.
- Efficacy in RRMS: Ocrevus has demonstrated substantial efficacy in reducing relapse rates among individuals with RRMS, marking a significant stride in MS management2.
- FDA Approval and Availability: Being approved by the FDA, Ocrevus has been a viable option for many individuals battling RRMS, offering a ray of hope in their treatment regimen.
What makes Ocrevus a reliable medication for MS?
Ocrevus boasts of established efficacy and safety data, having significantly reduced relapse rates, disability progression, and MRI lesions over 7 years of clinical trials and real-world use. This long-term data provides a sense of reliability and trust in its effectiveness in managing MS.
Besides the IV infusion, Ocrevus can also be administered through two subcutaneous injections, providing an added layer of convenience for patients who might prefer or require this method of administration.
What are the drawbacks associated with Ocrevus?
Ocrevus has a higher rate of infusion reactions, at 34%, which may necessitate pre-medication and observation, potentially leading to a more cumbersome treatment experience. The slower onset of action in depleting B cells and reducing disease activity compared to Ublituximab can also be seen as a drawback.
Additionally, the two-step dosing schedule of Ocrevus, requiring two separate infusions two weeks apart for each dose, might be seen as less convenient when compared to the single infusion required for Ublituximab.
Side-by-Side Comparison
This table encapsulates a snapshot comparison between Ublituximab and Ocrevus, highlighting their FDA approval status, mechanism of action, efficacy in RRMS, and brand names.
The journey of understanding and comparing these two potent therapies will be further explored in the subsequent segment, delving deeper into their comparative analysis, consumer insights, and original unique perspective in the broader MS treatment landscape.
| Parameter | Ublituximab | Ocrevus |
|---|---|---|
| FDA Approval Status | Approved | Approved |
| Mechanism of Action | Anti-CD20 Monoclonal Antibody | Anti-CD20 Monoclonal Antibody |
| Efficacy in RRMS | Under Evaluation | Reduced Relapse Rates |
| Brand Name | Briumvi | Ocrevus |
Comparative Analysis of Ublituximab and Ocrevus
The journey of understanding Ublituximab and Ocrevus takes us further into the realm of efficacy, safety, and cost. These factors are paramount when evaluating the potential of these therapies in the management of Multiple Sclerosis (MS).
Efficacy and Safety
Both Ublituximab and Ocrevus operate by targeting the CD20 protein on B-cells, pivotal in the inflammatory processes associated with MS. However, the extent to which they manage the disease varies.
- Relapse Rate Reduction: Studies have shown Ocrevus to be effective in reducing the relapse rate among RRMS patients. The efficacy of Ublituximab in this regard is under continual evaluation.
- Disability Progression: While both therapies aim at slowing down disability progression, the comparative data on their efficacy is yet to be robustly established.
- Side Effects: As with any therapy, understanding the side effect profile is essential. Common side effects associated with these therapies include infusion reactions, infections, and potential immunosuppression.
The journey of managing Multiple Sclerosis (MS) with the aid of Disease Modifying Therapies (DMTs) like Ublituximab and Ocrevus unveils a broader narrative. It's not merely about the reduction of relapse rates or slowing down disability progression; it's about enhancing the quality of life for individuals battling this relentless disorder. The inception of these therapies embodies a beacon of hope, offering a premise of more good days than bad, and a potential restoration of normalcy that's often disrupted by MS.
Availability and Cost
The accessibility and cost of DMTs are crucial factors that influence the choice of therapy for many individuals.
- Insurance Coverage: Insurance coverage significantly impacts the affordability of these therapies. It’s imperative to understand the insurance landscape surrounding Ublituximab and Ocrevus.
- Assistance Programs: Pharmaceutical companies often have assistance programs to help offset the cost. Exploring these options can provide financial relief to patients.
Cost Comparison
| Aspect | Ublituximab | Ocrevus |
|---|---|---|
| Cost per Infusion | $5,000 | $65,000 |
| Annual Cost | $100,000 | $130,000 |
| Insurance Coverage | Varies | Varies |
| Assistance Programs | Available | Available |
Consumer Analysis
Delving into patient-centric perspectives reveals a myriad of hopes, concerns, and experiences associated with these therapies.
Pros and Cons
- Benefits: Both therapies offer hope in reducing relapses and managing symptoms of MS.
- Risks: Awareness of potential side effects and the financial burden is essential for making an informed decision.
The emergence of Ublituximab and Ocrevus signifies a promising stride in the evolving landscape of MS treatment. Their unique mechanism of action targeting B-cells portrays a significant shift towards more targeted therapies in managing MS.
Frequently Asked Questions
Which is better rituximab or Ocrevus?
Both Ocrevus (ocrelizumab) and rituximab hold significant places in the treatment paradigm of Multiple Sclerosis (MS). However, Ocrevus has a slight edge due to its more selective targeting of CD20+ B cells and a longer duration of B cell depletion as compared to rituximab. Moreover, clinical trials have shown Ocrevus to demonstrate superior efficacy over interferon beta-1a, which makes it a more preferred choice among healthcare practitioners for managing MS.
Is Ocrevus the best MS drug?
The term "best" can be subjective as the effectiveness of MS drugs can vary from individual to individual. Nevertheless, Ocrevus has been recognized as one of the most effective MS drugs currently available. Its high efficacy in reducing relapse rates, slowing down disability progression, and mitigating brain lesion activity in both relapsing and primary progressive MS makes it a robust therapeutic option.
How is Ocrevus different from rituximab?
Ocrevus and rituximab, while similar in their mechanism of targeting CD20, have notable differences. Ocrevus is known for its more selective targeting of CD20, and it results in near-complete depletion of CD19+ B cells for an extended period of 6-9 months as compared to rituximab's 3-6 months. Moreover, Ocrevus requires a bi-annual administration, while rituximab may be administered every 6 to 12 months, making Ocrevus a more convenient option for many patients.
What is the difference between Briumvi and Ocrevus?
Briumvi (brisanlimab) is an investigational CD19 monoclonal antibody, whereas Ocrevus targets CD20. This difference in target may allow Briumvi to enable a more rapid repletion of immature B cells compared to Ocrevus. However, Ocrevus has a more robust clinical trial data backing its efficacy and safety, which gives it a reliable standing in the MS treatment landscape.
What is the strongest drug for MS?
Both Ocrevus and Lemtrada (alemtuzumab) are often cited as the most effective MS drugs currently available due to their potential to lead to no evidence of disease activity (NEDA) in a significant proportion of patients. Their strong efficacy in managing MS symptoms and preventing disease progression makes them formidable options.
What is the strongest treatment for MS?
Alongside Ocrevus and Lemtrada, hematopoietic stem cell transplantation (HSCT) is also considered a potent treatment for MS. These treatments have shown remarkable ability in reducing relapse rates, disability progression, and MRI lesion activity, thus standing as strong therapeutic options for MS patients.
Why is Ocrevus so good?
The efficacy of Ocrevus is largely attributed to its mechanism of depleting CD20+ B cells, which are believed to play a crucial role in MS autoimmunity and progression. Clinical data has shown that Ocrevus can reduce relapse rates by around 50% and disability progression by 40% compared to interferon beta-1a, which underscores its significant impact in managing MS.
What is the best infusion therapy for MS?
In the realm of infusion therapies for MS, Ocrevus and Lemtrada are often regarded as the most effective. While Ocrevus requires less frequent dosing, Lemtrada offers the potential for long-term drug-free remission in some patients, which can be a preferable outcome for certain individuals.
How successful is Ocrevus?
Clinical trials have demonstrated the substantial effectiveness of Ocrevus in managing MS. It has been shown to reduce annual relapse rates by around 50% and disability progression by 40% versus interferon beta-1a over a span of 2 years. Moreover, up to 80% of patients achieve a status of no evidence of disease activity after 2 years of treatment with Ocrevus, which speaks volumes about its success in the therapeutic arena










